Call 800-359-5690
Find a Location
Nursing Home Abuse & Neglect Lawyers
Texas has the highest percentage of one and two-star nursing homes in the country. Unfortunately, elder care facilities in the state have historically ranked lowest among all 50 states and the District of Columbia when it comes to providing adequate care for nursing home residents. In most instances, nursing home abuse and neglect stem from a statewide problem of understaffing. However, according to the Nursing Home Abuse Lawyers on our staff, understaffing is no excuse for inadequate care or abuse in nursing homes and other elder care facilities. Elderly patients who live in facilities with staffing issues often suffer from bedsores, sometimes called pressure sores, and falls. Call a Nursing Home Bedsore Lawyer or Nursing Home Fall Lawyer to discuss the specifics of your case.
The Carlson Law Firm has been representing nursing home residents and their families since 1976. Our firm has some of the top nursing home abuse attorneys in the country. We help families whose loved ones have been injured or killed from abuse and negligence in the following elder care facilities:
- Nursing Homes
- Assisted Living Facilities
- In-Home Care
- Adult Day Cares
- Continuing Care Retirement Communities
- Dementia Care Facilities
By proving that the staff in one of the above facilities subjected your family member to some form of elder abuse or neglect, you may be able to recover financial compensation for everything from medical expenses to damages for pain, suffering, and emotional distress. We serve victims of nursing home neglect and abuse and their families nationwide. No appointment is required and bilingual staff members are available to assist our Spanish-speaking clients. Contact The Carlson Law Firm today for a free, no obligation, case evaluation.
Nursing Home Bedsore Lawyer
Bedsores (also known as pressure sores and decubitus ulcers) are one of the more ailments for nursing home residents. However common doesn’t mean that bedsores aren’t preventable. When bedsores appear, it should be concerning as it is a major red flag that something isn’t right in your loved one’s care. When a nursing home resident develops bedsores, it is typically a sign of nursing home neglect. Bedsores can develop while the resident is lying in bed, sitting in a wheelchair or being otherwise immobile. Bedsores can be exacerbated by friction or excess moisture on the skin. If you suspect your loved one is suffering from nursing home neglect then contact The Carlson Law Firm to speak with a Bedsore Lawyer.
Once formed, bedsores are very painful, can take months to heal—if they heal at all. Bedsores can complicate existing health problems. It is not unusual for nursing home residents to die as a result of infections that develop from bedsores.
What are the risk factors for developing pressure sores?
Certain conditions may leave a person at greater risk for bedsores. The following are common risk factors that the nursing home MUST take into account when assessing and caring for a resident:
- Immobility. Often the result of fractures sustained during falls. However, any condition that impacts a person’s ability to move puts them at risk for pressure sores.
- Poor nutrition and hydration. The skin needs nutrition to remain healthy. Additionally, it needs proper nourishment to heal itself. If nutrition is inadequate, there is a greater risk for pressure sores because the skin is less resilient.
- Peripheral vascular disease. Poor blood circulation can occur from a number of conditions. These conditions include diabetes, heart conditions, and kidney diseases.
- Rubbing and/or Friction. If the skin constantly rubs against something else, you may be prone to pressure sores. For nursing home patients, this can happen when being moved in and out of a wheelchair or in just sheets on a bed.
What causes pressure sores?
Simply stated, pressure sores develop on the bony prominence of the body when there is continuous pressure on that area. Areas most at risk for pressure sores include the coccyx, hips, and heels. Still, other areas with unrelieved pressure are at risk as well. Immobile nursing home residents will likely develop bedsores if those charged with their care do not take consistent measures to reposition the resident and relieve pressure.
Other factors include:
- Shearing. Shearing occurs when the patient is in a bed that can be raised or lowered. In these cases, when a patient is in one position for a long period of time and quickly changes position, damage to the skin—and even the tissue—can occur.
- Friction. Constant rubbing against the skin can cause bedsores to develop. This is especially true if the skin is tender or wet. It is imperative that nursing home employees keep the fabric rubbing against the skin to a minimum. Additionally, they should ensure clothing and linens are dry and clean.
Whenever a nursing home fails to prevent bedsores, it could be a sign that your loved one is being neglected. If you suspect that your loved one is being neglected, contact a Carlson Law Firm Bedsore Attorney to discuss your case.
Necessary Bedsore Prevention Measures
Cleanliness
As mentioned above, cleanliness is also a key factor in preventing and healing pressure sores as well. When a resident is forced to lie in her own waste for hours, the acidity of the urine tends to break down the skin. This breakdown can lead to the development of bedsores or worsen an existing pressure sore. If a nursing home resident with one or more bedsores is forced to lie in their own urine or feces for hours on end (which, sadly, is a common event at nursing homes), there is the added danger of infection. Once bedsores become infected, the resident is in grave danger of developing a systemic infection throughout her body known as sepsis. Sepsis is very difficult to treat and often results in death.
Nutrition
Another key factor in the prevention and healing of pressure sores is hydration and nutrition. When a nursing home is understaffed or the staff is poorly trained, some of the most basic necessities of life are overlooked. For example, many immobile residents rely entirely upon the nursing home staff for the most basic of care, including giving them a drink of water or assisting with meals. When those basic staples are not accomplished, residents are at risk of becoming dehydrated and malnourished. Dehydration and malnourishment weaken the body. When a person is dehydrated, their skin becomes less supple and more brittle, making them more prone to the development of bedsores. A person who is malnourished has less fat and muscle, making it easier for bed sores to develop. Additionally, sores can worsen at a faster rate when a person is malnourished.
How are bedsores diagnosed?
Pressure sores are classified according to stages. Generally speaking, each stage of bedsores represents a greater degree of tissue and skin damage than the stage before it. Pressure sores can develop quickly and can become a serious problem very quickly. When blood flow circulation is compromised, affected tissue can die. This can cause an ulcerated sore to form.
There are four classifications of pressure ulcers that indicate the severity of the ulcer:
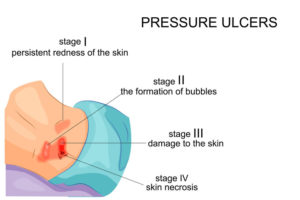
Stage 1: Presents as an area of persistent defined redness of the intact skin, usually over a bony prominence.
Stage 2: Presents as an abrasion or ruptured fluid-filled blister involving partial skin loss.
Stage 3: The wound is open where subcutaneous fat is visible; however bone, muscle and tendon are not visible.
Stage 4: Wound is deep with full-thickness tissue loss. Muscle, tendon, and bone are visible.
If your loved one is suffering from a later stage bedsore, you have a right to seek justice. Compensation is not the ultimate goal in nursing home cases—holding nursing homes to high standards is The Carlson Law Firm’s goal. It is important that at-fault parties are held accountable for their negligence of elderly and other nursing home patients. When you contact a Bedsore Lawyer from The Carlson Law Firm, we will fight to make nursing home experiences better for your loved one and future patients.
How should nursing homes prevent bedsores?
Without a doubt, pressure sores are easier to prevent than they are to treat. That is why nursing homes have many practices at their disposal to prevent pressure sores. By taking these steps, nursing homes can stop an existing pressure sore from worsening. For example:
- Keep residents well fed, well hydrated and kept clean and dry
- Change the position of residents who are bedridden or in wheelchairs regularly. Bed-bound patients should be moved at least once every two hours.
- Special mattresses can help alleviate the threat of pressure sores; however, these mattresses do not take the place of repositioning the patient every two hours.
- The use of special heel protectors and boots can help alleviate pressure to the affected areas.
We recognize that in cases where patients are bedridden or spend most of the day in a wheelchair, it can prove difficult to prevent bedsores from appearing. However, the staff still has a responsibility to take precautions to keep bedsores from even forming. For example, patients with severe immobility should be in physical therapy programs. This can help keep them moving and keep the blood flowing. Also, it will help stop atrophying from forming in the muscles. If patients are able to walk, nursing homes should allow and encourage them to do so.
Another preventive measure is to take include checking a patient’s skin regularly. If any signs of bedsores are noticed, the nursing home staff should immediately take measures to correct the issue. By keeping patients and their linens clean and dry, nursing home staff can lessen the chances of bedsores progressing. Foam pads on the bedding can provide more comfort and cushion to areas prone to developing sores.
If a nursing home failed to protect your loved one, contact our Bedsore Lawyer today for a free consultation.
Nursing Home Fall Lawyer
Nursing home falls represent 36% of preventable emergency room visits among nursing home residents. However, The Centers for Disease Control and Prevention (CDC) reports that nursing home falls go largely unreported. But, even with underreporting, the CDC receives between 100 and 200 reports of nursing home fall every year from average-sized nursing homes. When these injuries happen, they can lead to devastating disabilities for elderly residents. If you suspect nursing home neglect and abuse, contact a nursing home fall lawyer to discuss your loved one’s reduced quality of life after a fall.
What happens when an elder person falls in a nursing home?
According to the Centers for Disease Control and Prevention, 1,800 nursing home residents die from fall-related injuries every year. Those who survive often suffer debilitating injuries from which they never fully recover. However, family members of loved ones in elder care facilities should know that falls are often preventable—as long as employees take the proper steps to supervise and protect residents under their care.
Common causes for falling in nursing homes include:
- Elderly residents have difficulty walking due to muscle and bone density loss
- Medication side effects
- Vitamin D deficiency;
- Foot pain
- Poor footwear
- Uneven steps
- Cognition problems
- Blood pressure
- Poor vision
- Walking and balance problems
Nursing home falls frequently cause a disability, functional decline, reduced independence, and reduced quality of life for an elderly person. Patients with a fear of nursing home falls may also experience feelings of helplessness, loss of function, depression, anxiety, and social isolation. Because of these life-altering injuries, nursing home staff have a responsibility to prevent falls. When they are negligent in their duties, a qualified nursing home fall lawyer can help you hold them accountable.
Are Elder Care Facilities Liable Injuries?
It is important to note that not every fall is preventable. Additionally, not every injury will lead to a viable personal injury lawsuit. However, this shouldn’t deter you from seeking a free consultation with a qualified Nursing Home Fall Lawyer. There are plenty of cases, particularly in Texas, that can be attributed to negligence as a result of understaffing. For example, as many as one-quarter of nursing home falls are because of environmental hazards such as wet or slippery floors. By contacting a qualified nursing home fall lawyer, we can help you determine if the nursing home was negligent or failed to prevent a fall. While this a broad net to cast, the following are examples of likely liability:
- Failure to develop an adequate fall prevention plan
- Improper care techniques
- Failure to assess, reassess or modify the resident’s care plan
- Understaffing
- Hiring unqualified employees
- Providing insufficient training
- Failure to address hazardous conditions such as wet floors, inadequate lighting and defective flooring
- Failure to provide care in accord with the fall prevention plan
This is not an exhaustive list of the kind of negligence that can occur in nursing homes. A nursing home fall lawyer can help you determine whether or not you have a viable personal injury lawsuit. If you believe you or your loved one was injured as an act of negligence contact The Carlson Law Firm as soon as possible.
Here at The Carlson Law Firm, we have a group of highly educated and well-respected Nursing Home Abuse and Neglect Attorneys on staff. Our attorneys are known across the nation for their efforts in prosecuting claims of negligence, neglect, and abuse in nursing homes and assisted living centers around the country. Pursuing these types of cases requires experience, knowledge, professionalism, and drive – all of which our nursing home attorneys have plenty of.
Protecting Your Loved One
According to the latest data, there are more than 15,000 nursing homes in the United States. In fact, as many as 52% of adults who reach age 65 will need long-term care in their lifetime. Currently, there are over 3.2 million adults living in long term care and nursing home facilities nationwide. With high numbers like these, the reality of nursing home neglect is that much more frightening.
Nursing home mistreatment can increase residents’ chance of death by 300 percent in the first three years following the abuse.
An important step in protecting the rights of our elderly loved ones is to learn the dozens of warning signs associated with nursing home abuse and neglect. With this knowledge, you’ll hopefully be able to help your loved one before the problem progresses.
- Weight Loss: While medication can affect a person’s appetite, this isn’t the only cause of weight loss in elders. Nursing home facilities are responsible for ensuring that all residents receive the necessary nutrition and hydration they need to maintain a healthy weight and remain in good health.
- Bruises: Similar to weight loss, certain medications can make a person more susceptible to bruising, but bruising is rarely accidental. If you notice bruises in patterns or clusters, or bruises that re-appear, this can be the sign of intentional bruising. A study in the Journal of American Geriatrics Society, Bruising as a Marker of Physical Elder Abuse, reported that bruises occurring as a result of physical elder mistreatment are often large and occur on the face, lateral right arm, and back of the torso.
- Reclusiveness: You probably know your loved one better than anyone else. If you notice that they are becoming less social and are experiencing mood swings, it may be a result of elder abuse or neglect.
- Poor Living Conditions: Sometimes evidence of nursing home abuse does not directly deal with your loved one, but rather the state of the conditions they reside in. Check out their room for bed bugs, unsanitary bathroom stalls, or cracked windows for example. If a nursing facility fails to maintain their facilities, you can almost guarantee they are also failing to maintain the standard of care for your loved ones that you expect.
Nursing Home Abuse Makes Headlines, Nursing Home Neglect Takes Lives
Nursing home neglect is the quieter cousin of nursing home abuse. Unfortunately, nursing home neglect happens far more frequently than many people realize. Elder neglect can be intentional or unintentional, but in either case, it’s still a form of elder abuse.
In most cases, nursing home neglect occurs because of understaffing. An understaffed facility means that there are not enough staff on duty to care of the patients.
Nursing Home Abuse Cases We Handle
The Carlson Law Firm has a core value to protect the most vulnerable populations. Bedsores are a serious condition that can lead to lifelong pain and even death. In fact, bedsores are the underlying cause for the death of several thousand people in the country every year. Our firm employs attorneys who are 100 percent dedicated to fighting for the rights of nursing home patients. A Bedsore Lawyer from The Carlson Law Firm will invest our time, legal expertise and resources to recover damages.
When it comes to burns and fire injuries, elderly are at a far greater risk. Some of the important factors to consider here are a decrease in mobility, hearing, and diminished eyesight. These contribute to a delayed response and could end up costing residents their lives.
The most common manner in which nursing home residents are burned is when they are bathed in scalding water in the nursing home. Regardless of the manner, burns to nursing home residents can be painful, severe, and even life threatening. If a nursing home resident suffers burns it may very well be due to negligence on the part of the nursing home.
Scalding
The skin on elderly individuals is fragile. In a sense, it is just as fragile and tender as a newborn baby. Consequently, when giving a bath to an elderly nursing home resident, nursing home employees must be cognizant to the vulnerabilities associated with the resident. Sadly, many residents suffer serious burns after being submerged in scalding water.
Smoking Accidents
The skin on elderly individuals is fragile. In a sense, it is just as fragile and tender as a newborn baby. Consequently, when giving a bath to an elderly nursing home resident, nursing home employees must be cognizant to the vulnerabilities associated with the resident. Sadly, many residents suffer serious burns after being submerged in scalding water.
How We Can Help
If a resident in a nursing home is hurt by a serious or fatal burn injury because of nursing home abuse or negligence, the resident and their family have the right to seek to hold the facility and its staff accountable for their wrongs. Nursing home lawsuits don’t just help victims of abuse and neglect recover compensation for their damages, but also act to send a message to nursing home and extended care facilities that the law will protect seniors, and see to it that abuse and neglect will be punished.
Burns remain one of the most painful and debilitating type injuries. When burns are caused by the carelessness of others, a nursing home patient is entitled to recover compensation from the facility where the burn occurred. If you believe that a loved one may be the victim of nursing home neglect or abuse you should take action quickly and contact us to set up a free consultation. Contact The Carlson Law Firm to speak with a nursing home Burn Lawyer 24 hours a day, 7 days a week.
For many people living in a nursing home facility, swallowing food may prove difficult. This means that nursing homes have to monitor or supervise the food intake of its patients. The risk of choking, possibly even death, increase when nursing homes fail to enforce diet restrictions or do not pay close attention to those patients who are susceptible to problems with choking.
Nursing home residents often have medical problems or take medications that make it difficult to properly chew or swallow food. Due to this, many are at high risk for choking.
The reason that many elderly and disabled patients have problems swallowing is varied. There 50 pairs of muscles and nerves involved when it comes to swallowing food, there are many conditions that may influence whether that patient is able to swallow or not. Some of the most common disorders include:
- Neurological Disorders – Neurological disorders such as Parkinson’s disease, muscular dystrophy, and multiple sclerosis may all influence the ability to swallow.
- Neurological Damage – If a person has suffered spinal or brain injuries or has suffered a stroke, it may affect his or her ability to swallow.
- Cancer – There are types of cancer that may affect the patient’s ability to swallow. The radiation treatment may also play a role here.
- Alzheimer’s Disease – Alzheimer’s patients in the later stages of the disease may find it difficult to swallow and eat.
- Aging – Considering it takes 50 pairs of muscles and nerves to swallow, it is not surprising that wear and tear on the throat muscles can make it difficult to swallow for older patients.
Choking Injuries
Choking, by depriving oxygen to the brain, can cause brain damage, and even death. While such an injury may appear to be accidental, in some instances choking is a result of nursing home neglect. When this is the case, it is important that nursing homes are held accountable for their fatal mistakes.
If the choking occurred because the patient was fed the wrong food or was not properly monitored, it is the fault of the nursing home, and your loved one may have a nursing home abuse lawsuit.
Choking Prevention
It is standard for those patients who have trouble swallowing in a nursing home setting to be examined by a physician in order to determine the severity of the problem. From there the physician can make recommendations on what the patient should and should not eat and in which forms. It is important that this advice be placed on the nursing home patient’s chart; these special needs need to be known to all caregivers who interact with the patient. When not monitored closely or if the patient receives medication or food that goes against what the physician recommended, it may lead to choking and asphyxiation.
How We Can Help
If you believe that a loved one may be the victim of nursing home neglect or abuse you should take action quickly and contact us to set up a free consultation. We are available to speak with you 24 hours a day, 7 days a week.
When nursing homes fail to implement proper precautions to address a resident’s risk for falls, and the resident is injured, family members should take action. Although some falls are unavoidable, oftentimes falls in nursing homes are a sign of nursing home negligence. We have handled many cases where residents have suffered serious injuries as a result of under-staffing in long-term care facilities. When staff cannot properly supervise monitor residents, fall-related injuries are more likely to occur.
Nursing home staff plays an important role in protecting the safety of residents as they move about the facility. When a patient is admitted into a nursing home, staff must assess his or her risks for falls and identify and implement interventions to address these risks. Reassessments should occur after any fall or change in medical condition. Residents at risk should be monitored closely and receive assistance with transfers to prevent them from falling. Bed rails, non-skid footwear, appropriate armchair with wheels locked at the bedside, walkers and canes can be used to help prevent falls.
If you believe that a loved one may be the victim of nursing home neglect or abuse you should take action quickly and contact us to set up a free consultation. Our Nursing Home Fall Lawyers are available, 7 days a week.
Maintaining appropriate nutritional and hydration status is important in the nursing home setting. Residents who do not receive adequate nutrition and hydration in their diets are more at risk for the development of pressure ulcers, infection, muscle weakness leading to immobility and falls and poor nutrition and hydration make it more difficult for existing pressure ulcers and infections to heal.
The elderly have less water content in their bodies than younger adults and a decreased thirst response which, among other factors, puts them at risk for dehydration. Increasing fluid intake in the elderly is important and relatively simple. The nursing home should monitor the resident’s fluid intake and ensure that the resident drinks at least six cups of fluid each day. Fruit juices, popsicles and gelatin are excellent sources of fluid which help residents maintain appropriate hydration.
There are a variety of factors which can lead to malnutrition. Depression, an increasing problem among the elderly, is a potential cause of malnutrition because individuals suffering from depression have a tendency to eat less and in turn do not receive appropriate vitamins and minerals to prevent malnutrition. Other causes of malnutrition include difficulty swallowing and adverse drug effects such as vomiting and diarrhea. Nursing homes often fail to take steps to prevent malnutrition by not monitoring resident food intake and output, not providing a comfortable environment to promote eating and not providing food that is appetizing.
How Do I Recognize Malnutrition Or Dehydration In My Family Member?
Sometimes changes can be subtle and if you visit your loved one every day, you may not notice gradual changes. In addition to periodically doing a thorough examination of your loved one for bruises and wounds, you should check them for signs of dehydration and malnutrition.
Common Signs of Dehydration
- Thirst
- Darker and more concentrated urine
- Fatigue
- Decreased urine output
- Light headedness / dizziness
- Muscle cramps
- Nausea and vomiting
Common Signs of Malnutrition
- Significant weight loss
- Fatigue
- Light headedness/dizziness
Residents in nursing homes are especially vulnerable to physical and sexual abuse. Tragically, reports of deliberate physical abuse, such as hitting, slapping, biting and attacks by other residents and even staff members are all too common. Nursing home residents are also victims of sexual assault in nursing homes.
The physical abuse of a nursing home resident can take on many forms, including beatings, biting, food or water deprivation, the inappropriate use of restraints, as well as over-medicating patients to keep them quiet, docile and easier to control. In some instances, physical abuse may manifest itself obviously in bruises, broken bones or cuts. Other times, physical abuse may not be as obvious.
What Does Elder Abuse Look Like?
Elder abuse is fairly straightforward. It is defined as intentionally acting in a way that results in the harm or risk of harm to an elderly person. You may not always know when your loved one has been physically assaulted in a nursing home setting. For example, patients with dementia or other medical conditions may be unable to tell someone what happened to them. Other times, victims fear that the perpetrator will beat or injure them again if they speak up. Sometimes, generational ideas like being seen as a burden or a problem for others can hinder a victim of nursing home physical and sexual abuse from speaking up.
The physical abuse of a nursing home resident can take on many forms, including:
- Beatings, including slaps, punches, hitting with objects, kicks
- Threats involving guns, knives or other weapons
- Biting
- Food or water deprivation
- Inappropriate use of restraints
- Use of over-medicating patients to keep them quiet
- Docile and easier to control
In some instances, physical abuse may manifest itself obviously in bruises, broken bones or cuts. Other times, physical abuse may not be as obvious.
Elder sexual abuse is the initiation of physical or sexual contact with an elderly person. In these cases, the contact is usually non-consensual or unwanted. This includes sexual contact with an elderly person who is confused or unable to give consent. Unwanted touching or rape are examples of nursing home sexual abuse.
Types of nursing home sexual abuse include:
- Unwanted touching
- Sexual assault and battery
- Sexual assault and battery
- Forced nudity
- Sexual photography
- Rape
How We Can Help
Because elder abuse is a growing problem, lawyers are finding themselves in the position to represent unsuspecting families. Nursing home physical abuse and nursing home sexual abuse can leave you questioning if you failed in protecting your loved one. You didn’t. It is an unfortunate reality that no amount of research or recommendations on a long-term care facility or nursing home can prevent your loved one from being abused or fatally injured. We believe we have a duty to protect our most vulnerable populations. By contacting The Carlson Law Firm, you are doing more than seeking compensation—you are seeking justice. Together, we can help improve the conditions of nursing homes across the country. Our firm has a nursing home physical abuse attorney that can help you prove that the nursing home you trusted physically abused and assaulted your loved one. We can help you get justice.
If you believe that a loved one may be the victim of nursing home neglect or abuse you should take action quickly and contact us to set up a free consultation. Someone from our team is available to speak with you 24 hours a day, 7 days a week.
Medical staff uses endotracheal tubes, or breathing tubes, to open a patient’s airway and increase oxygen intake. The tubes are usually attached to ventilators, or breathing machines, to keep oxygen intake consistent. If a nursing home doctor, nurse or other staff member fails to properly insert or monitor the tube, serious suffocation and choking risks can arise.
If your loved one experiences breathing difficulties due to medical conditions such as pneumonia, asthma or COPD, he or she may require the occasional short-term use of breathing tubes and ventilators. Even if your loved one does not have one of these conditions, staff may need to insert a breathing tube into his or her trachea, or wind pipe, for one of the following reasons:
- To increase the amount of oxygen your loved one takes in
- To clear mucus out of your loved one’s lungs
- To keep your loved one’s wind pipe open
If your loved one continues to experience breathing difficulties, his or her care staff may choose to remove the breathing tube and perform a tracheotomy. This procedure involves creating a small hole in the neck that will keep the airway open.
How a Breathing Tube Gets Clogged
Food can enter the tube from either end. Saliva or phlegm may also find its way in. Under normal care and supervision, staff would remove any obstruction and no harm would occur to your loved one. However, in situations where a nursing home is understaffed or the existing staff is negligent, either by design or through improper training, these obstructions can lead to oxygen deprivation or cardiac arrest. Severe clogged breathing tube cases lead to permanent brain damage, early mortality and even death.
Clogged breathing tubes, similar to choking, can cause brain damage, and even death because the brain is deprived of oxygen.
While such an injury may appear to be accidental, nursing homes can be held accountable. If the choking occurred because the patient was not properly monitored and this led to a clogged breathing tube, it is the fault of the nursing home, and your loved one may have a nursing home abuse case.
Maladministration of medicine and medication errors are frequent and serious problems at nursing homes. Residents are given the wrong medication or not given the medication in the dosage or frequency as required by the physician’s order. This occurs as a result of carelessness on the part of the staff, lack of supervision of the nurses administering the medications or not having enough properly trained and supervised to staff to administer the medications.
Studies have shown delayed or missed treatment or medication and the administration of the wrong dose or the wrong medication are the two most common medical mistakes made in the hospital setting. Studies also show that nursing home medication error occurrences are widely under reported. It is estimated that only 1.5% of all medication errors are actually reported.
Nursing home and medication error risks can be considerable because many patients are on a number of prescriptions and have already compromised physical health conditions. These risks are also exacerbated by the fact that nursing homes are often understaffed. If medication error causes injury to a resident, they have the right to seek compensation for their losses.
Examples of Medication Errors
To the untrained eye, it may be difficult to determine whether something qualifies as a medication error. However, once you have a better understanding of what constitutes a medication error, it is easier to be aware of them.
- Splitting medications that should not be split – These include tablets, capsules, or other types of medication that specifically say, “Do not crush.”
- Not having enough fluid – There are countless prescription medications that require the elderly patient to consume a certain amount of fluid when ingesting the medication. Improper hydration or not taking in fluid when taking the medication may actually cause harm to the patient.
- Inadequate antacids or food – Just as some prescriptions require fluid, others require food. There are also medications that require the patient to take an antacid before ingesting the medication. It is important that the nursing staff ensure that patients follow the recommended guidelines regarding antacids, fluids, and food.
- Not preparing the medication properly – There are a number of nursing home medications that require that it be shaken or mixed before the patient takes it. Without following the proper procedure, the resident is at risk of receiving too much or too little of the medication. For example, it is important to mix insulin suspensions without air bubbles before administering the medication.
- Swallowing sublingual tablets – Sublingual tablets are administered by placing them underneath the tongue and allowing them to dissolve. However, some elderly patients will swallow these sublingual tablets instead. While once or twice might not be terrible, it is important that the staff recognize this is happening and address this as a reoccurring issue. Perhaps the medication needs to be altered to ensure proper ingestion.
The Nursing Home Reform Act of 1987 gave all nursing home residents the right to be free from restraints when the restraints are used for disciplinary purposes or for the convenience of the nursing home corporation. Restraints can be either chemical (i.e., medication designed to make the resident passive) or physical. Regardless of the type of restraint sought, they must be ordered by a doctor. Restraints used without a physician’s order are illegal.
Chemical restraints are usually antipsychotic drugs that are used by the nursing home to control individuals who suffer from dementia or anxiety. For a nursing home focused primarily on reducing its budget and operating on minimal staff, chemically restrained residents are easier to control and require less care than active residents. In fact, staffing shortages are a leading culprit in explaining why some nursing homes choose to restrain residents.
A physical restraint is usually a device placed next to or around a resident to limit or eliminate movement by the resident. One of the most common examples of a physical restraint is the side rail on the bed. Designed to prevent a resident from falling out of bed, side rails can sometimes do more harm than good. Some of the most common injuries with side rails are falls when an unmonitored resident attempts to crawl over the side rail or asphyxiation when a resident becomes entrapped between the mattress and the side rail. Nursing homes are supposed to evaluate residents for these known dangers and supervise accordingly. When they choose not to, the resident is at great risk for serious injury or death.
Physical Restraint Injuries
Physical restraints restrict an individual’s movement in some way. Physical restraints commonly used in nursing homes include:
- Wrist and ankle restraints
- Hand mitts
- Bed rails
- Vests tied to beds or chairs
Chemical Restraint Injuries in Nursing Home
In nursing homes, psychoactive drugs are the most common types of chemical restraints given to residents who are uncooperative or restless. Using these types of drugs in such an unethical manner can have devastating consequences. Because of chemical restraints, the patient may do any of the following:
- Become confused
- Become disoriented
- Be unable to carry out the tasks of daily living
- Become agitated
- Experience an overall decrease in quality of life
Effects of Improper Use of Restraints
Although you will not be able to monitor the actions of nursing home staff around the clock to ensure that they are, in fact, properly using restraints, knowing the signs of improper use of restraints can help you identify when or if your loved one may be the victim of nursing home abuse. Some indications of the improper use of restraints can include:
- Physical injuries, such as bedsores or wrist and/or ankle damage
- Diminished mental capacity, such as disorientation, depression or an inability to process thoughts, when chemical restraints are being used.
Sepsis is a severe infection caused by bacteria in the tissue or blood stream. Properly treated, an infection is usually localized and curable. When left untreated, a minor infection can increase in intensity and scope to the point where the entire body suffers from a systemic severe infection. At this point, the infection is often referred to as sepsis or septicemia and is life-threatening.
Persons with this infection may experience fever, chills, loss of appetite, rapid breathing and irregular heartbeat. Many times, sepsis develops at the same time as infection in another part of the body, such as a respiratory, skin, or gastrointestinal infection. Sepsis may also coincide with or precede meningitis, an infection of the central nervous system. In severe cases, the infection can lead to infections of the brain and the heart, and subsequent death.
The skin is one of the main sites of infection. Normally, the skin serves as a barrier against all manner of viral and bacterial threats, but any cut or other open wound can allow a bacterial infection that can cause sepsis to develop. These include surgical sites, points of entry for intravenous lines, and sites of skin breakdown such as decubitus ulcers or bedsores.
Prevention can in part include monitoring the skin for the development of bedsores, and taking steps to prevent bedsores from developing. If sepsis develops in a patient who was improperly monitored or treated, the medical professionals in charge of administering care may be held liable.
This illness can kill patients who otherwise might have recovered fully from their original injuries or illnesses.
Wandering and Elopement are related concepts. Wandering refers to aimless movement throughout the facility where the resident puts his safety at risk due to an inability to appreciate danger. Elopement refers to the resident’s ability to leave the facility unsupervised and unnoticed putting the resident’s safety in danger.
What Should Nursing Homes Do To Protect Residents From Wandering and Elopement?
Nursing homes are required to assess each resident to determine their risk for wondering. If the risk is there, the facility is to initiate a plan of care specifically designed to care for the residents at high risk for wandering and elopement.
Some aspects to such care plans include:
- To consistently monitor doors—especially during shift changes where residents are particularly inclined to wander
- Place residents that have been characterized “at risk” for wandering closer to nursing stations so that they can be more closely monitored
- Using alarms on the resident’s bed, wheelchair or door as well as the residents themselves
- Exit doors should be alarmed to notify staff when residents leave the facility
Nursing homes must acknowledge the risks associated with patient wandering and elopement and take steps to minimize incidents from occurring in the first place. When facilities fail to implement preventative measures, they may be held responsible for the resulting patient injuries. Our nursing home attorneys know the feeling of guilt that may arise after a loved one suffers an injury at a facility and always take steps to minimize the impact on you and the rest of your family while aggressively pursuing the case. If your loved one was injured after leaving the safety of a skilled nursing facility, we are interested in speaking to you. Our attorneys know how to prosecute nursing home wandering cases and look forward to doing so for you. Call us anytime to discuss your legal options.
Wrongful death occurs when the negligence or carelessness of one person causes the death of another. The Carlson Law Firm has extensive experience in handling wrongful death cases associated with medical malpractice and nursing home abuse and neglect.
Nursing home residents almost always require the care of professionals for daily living needs, medical needs, or cognitive needs, which is why they are in nursing homes in the first place. However, when wrongful death occurs, it happens in the very hands of the professionals who were entrusted to take care of these elderly residents. This can result from a variety of issues, and the underlying problem behind the majority of issues is nursing home abuse and neglect.
Who Can Bring A Claim?
The laws on who can bring a wrongful death claim vary from state to state. In some cases, the wrongful death claim belongs to the surviving immediate family members. Other states require that an Estate be opened in the name of the deceased individual. Either way, having an attorney experienced in preparing and pursuing wrongful death cases is crucial.
How Is Compensation Handled In These Cases?
Survival statutes can give family members peace of mind in standing up for the legal rights of a loved one after death. Through a wrongful death statute, a cause of action survives the life of a deceased person. This means that if your loved one experienced neglect or abuse in a nursing home and later died, then you can still file a nursing home wrongful death lawsuit after the death of your loved one. Surviving family members can recover compensation that can be used to pay for outstanding medical bills and funeral expenses. In some cases, economic damages or damages for loss of companionship may also be available. Each state has its own Wrongful Death statute that specifies the total amount of damages that may be awarded to family members after the death of a loved one.
Assisted living is a hybrid between a retirement community and a nursing home. These facilities provide care for elderly people—or young people living with disabilities—who are unable to live independently but do not require the same level of care found in nursing homes. While the standard of care may be different than it is in a nursing home, many of the residents in assisted living facilities still suffer from certain health conditions that can impair both their physical and cognitive abilities to care for themselves. Assisted living negligence is a very serious risk to the well-being of those in need of the care these facilities have to offer. These facilities are required to ensure a resident’s quality of life doesn’t suffer. If you believe your loved one may be experiencing abuse or neglect, contact an Assisted Living Facility Negligence Attorney from The Carlson Law Firm.
The Carlson Law Firm has more than 40 years of experience representing victims and their families through the aftermath of personal injuries. Our compassionate attorneys understand that any form of neglect or abuse in assisted living facilities may be difficult for family members and loved ones to face. But the fight for justice has never been an easy one. Our legal team has some of the leading legal experts in elderly care neglect. You have the power to hold negligent parties responsible and prevent others from suffering in the same way your loved one has.
What Type Of Negligence Occurs In Assisted Living Facilities?
Residents of assisted living facilities are still vulnerable to the same of abuse and neglect as those who are more dependent on nursing home care. These facilities often don’t receive the level of scrutiny that nursing homes do. But seniors and other dependents in these facilities are still at risk of experience abuse, neglect, and negligence.
Assisted living facility negligence and abuse can take form in several ways:
Physical abuse
Occurs when there is harmful contact such as slapping, hitting, pushing or kicking. This form of abuse also includes excessive or improper use of restraints. In some cases, it may take form as the withholding of food or forcing a resident to consume food or drinks.
Psychological abuse
This type of abuse occurs when there is verbal assault, harassment, bullying, humiliating or degrading treatment of a resident. Giving a resident the silent treatment, or denying the resident of communication as a punishment is also a type of psychological abuse.
Isolation
Preventing or restricting visits from family and friends or preventing contact by telephone, mail, email or other means that isolates a resident from a loved one is abuse.
Neglect
Neglect is tricky to recognize. This is because it often doesn’t occur with malicious intent, but rather occurs as a result of understaffing. In other cases, it may occur as a result of staff indifference to the well-being of residents. Signs of neglect include unsanitary living quarters, dehydration, malnourishment or immobile injuries such as rashes and sores.
Financial exploitation
This type of elder abuse is often the subject of tabloid headlines or the plotlines of movies when a will is changed to exclude children in favor of a new spouse. However, taking financial advantage of a person can happen in any income threshold. Financial exploitation may occur when checks, money or property are stolen or their belongings such as vehicles are used without permission. Financial exploitation can worsen a person’s condition by leading to bills going unpaid.
These abuses may not just be carried out by staff, but also by other residents and even family members. They cause significant harm to seniors. Assisted living negligence that is allowed to persist is a violation of your loved one’s rights. Contact a qualified Assisted Living Facility Negligence Attorney to discuss your situation. You may be able to recover financial compensation.
What Are The Signs Of Assisted Living Facility Negligence?
Often, loved ones suffering abuse in these facilities are scared to come forward with the abuse or neglect they are experiencing. They may be ashamed or fear that the offender may retaliate in some way. Because of this, family members and loved ones must know what to look for when their loved ones are in an assisted living facility. The types of signs to look out for include the following:
- Broken bones or fractures
- Unexplained weight loss
- Bruising, cuts or welts
- Bedsores
- Frequent infections
- Dehydration
- Mood swings
- Emotional Outbursts
- Reclusiveness
- Refused to Speak
- Refused to eat
- Unexplained weight loss
- Refusal to take medications
- Poor physical appearance
- Lack of cleanliness
- Changes in mental status
- Caregivers do not want the patient left alone with others
- Noticeably strained relationships with others in the facility
- Sudden death
In the longterm care industry, negligence can often lead to serious health conditions. Neglect can open the door to several reasons to file a lawsuit, including a wrongful death lawsuit. If you spot any of the signs, you must take immediate action.
Why Does Assisted Living Facility Negligence Occur?
One of the biggest reasons neglect occurs in longterm care facilities is because of understaffing. As a result, some elderly residents end up being neglected. Understaffing can lead to significant oversight in a person’s care. For example, residents may not receive:
- Appropriate medication
- Scheduled meals
- Medical care
To combat understaffing, longterm care facilities may hire inexperienced staff that may not be as diligent in caring for residents.
Further, elderly citizens are entitled to living with dignity and respect. If your loved one is being treated unjustly in an assisted living facility, contact an Assisted Living Facility Attorney from The Carlson Law Firm to discuss your options.
Protecting Loved Ones From Abuse And Neglect
Finding out or suspecting your loved one is being abused or neglected is your worst nightmare. No one would ever put their loved one into a facility that would lead to their suffering. The awful headlines splashed across newspapers and evening news already make many people hesitant to put their loved ones in any facility. However, there are times when you don’t have the time or know-how to care for your loved one truly.
Above, we’ve discussed the warning signs to watch out for while your loved one is in the care of an assisted living facility. But it’s also crucial that you know what to do if you suspect that your loved one is being abused or neglected. Seniors have a right to be from abuse, neglect, and exploitation.
Protect your loved one by doing the following:
- Call and visit often
- Offer to stay and help on a regular basis to ensure your loved one is receiving proper treatment
- Monitor your loved one’s medication
- Keep an eye on their finances
- Identify warning signs of abuse or neglect
If you suspect that abuse or neglect is occurring, consider the following actions to protect your loved one:
- If your loved one is in immediate danger of physical or mental abuse, contact your local police department. Elder abuse and neglect are criminal matters that fall under police jurisdiction.
- Call your state’s governing body over nursing homes or assisted living facilities to report incidences of abuse or neglect. In Texas, this is the Department of State Health Services.
- If the victim receives Medicaid, report the longterm care facility to your state’s governing authority on fraud, waste and abuse. Or you can report it to the U.S. Department of Health and Human Service Office of Inspector General.
- Hold the facility accountable by contacting a qualifed Assisted Living Facility Negligence Attorney.
Ultimately, the best way to protect your loved one is to speak up. In most states, if you are aware of a specific act of elder abuse, the law requires that you report it.
Our Nursing Home Abuse Lawyers
Nursing Homes Should Be Staffing to Acuity
There is no magical number that nursing homes should have on staff. However, Carlson Law Firm Nursing Home Neglect and Abuse Lawyer, J.T. Borah says that nursing homes should be staffing to resident acuity. Staffing to resident acuity essentially means that clinical expertise and clinical resources are properly allocated depending on residents’ needs.
It can be extremely frustrating for families to discover that their loved ones are being mistreated at a facility that they trusted. Whether intentional or not, elder abuse is elder abuse. You need a qualified Nursing Home Abuse and Neglect Attorney on your side. The Carlson Law Firm’s Nursing Home Abuse and Neglect team are leaders of their field.
Contact a Nursing Home Abuse and Neglect Lawyer
Contact us today at 866-351-4092 to schedule a free consultation with a nursing home abuse and neglect lawyer. A nursing home abuse and neglect lawyer from The Carlson Law Firm is ready to assist you when a loved one has been harmed by the intentional or unintentional negligence of a nursing home.
There's a Carlson Law Firm Near You
With over a dozen locations throughout Texas, there’s a Carlson Law Firm near you. We have law offices located in Killeen, Temple, Waco, Round Rock, Austin, San Antonio, Kerrville, Laredo, Bryan, Lubbock, Midland, and Corpus Christi.
