Since the mid-2000s, HIV research has focused on ways to prevent the sexual transmission of HIV as a form of treatment. In September 2017, the Centers for Disease Control and Prevention adopted the widely accepted scientific position that an HIV-positive person with an undetectable viral load in their blood has a low risk of transmitting the virus through unprotected sex. Advancements in HIV treatment has dramatically improved the health, quality of life and life expectancy of people living with HIV. Additionally, these advancements have also transformed the HIV prevention landscape.
Scientists estimate that HIV spread from chimpanzees to humans in the early 1900s. Then, in 1968, the earliest suspected case of AIDS appeared in St. Louis, Missouri. By the 1980s, following the 1981 death of Gaetan Dugas, HIV/AIDS became an epidemic. In the early years, doctors were baffled about the virus that was making gay men in urban areas sick. From the government‘s slow and counterproductive response to Bayer being responsible for infecting millions of hemophiliacs with HIV, what unfolded throughout the 1980s laid the foundation for the preventative measures and medical advancements seen today.
While it is true that science has changed the way we treat HIV, attitudes about the disease have also come a long way from the panic and fear that gripped the United States in the early years. In fact, many people no longer take the threat of contracting the disease serious. This is because current medication is so effective in preventing full-blown AIDS and prolonging life. Billions of dollars and brilliant minds have been dedicated to finding a cure for HIV/AIDS. While a cure has yet to come to fruition, the advancements in technology have made the disease a manageable one, but manageable does not mean an HIV infection won’t completely change your life.
What is an ‘Undetectable’ Viral Load?
A person living with HIV has an undetectable viral load when antiretroviral treatment (ART) has brought the level of virus in their body to such low levels that blood tests cannot detect it. This medical advancement is a far cry from the early years of HIV when the disease sent panic rippling through the gay community and beyond.
The virus affects all sexual orientations, genders, races and income levels. Because of this, everyone has a responsibility to protect themselves when engaging in risky behavior.
HIV Treatment as Prevention (TasP)
With the CDC’s 2017 declaration, the effectiveness of ART as a prevention tool is now undisputed. Around the globe, health agencies are adopting treatment and prevention to curb HIV infections. This is because studies, such as the 2016 Partner Study, show that HIV positive people on an effective ART with an undetectable viral load have negligible chances of transmitting HIV to others. The World Health Organization (WHO) believes that ‘test and treat’ strategies—administering ART as soon as possible after diagnosis—will ultimately decrease the rate of new HIV infections.
After beginning ART, it takes about six months for an HIV positive person to reach undetectable levels. Also, with the use of pre-exposure prophylaxis (PrEP), people at the highest risk for HIV can take daily medications to lower their chances of infection. With proper condom use, antiretroviral treatment and PrEP puts the chances of contracting HIV from a positive partner at nearly zero.
“Effectively No Risk”: What the CDC says about undetectable viral loads
Years of studies and billions of dollars of research have culminated in effective HIV treatment and prevention. While these new medications are not a cure for those already infected by the virus, they have a significant effect on reducing the likelihood of transmission. The CDC has taken the stance that treatment as prevention is the best way to end the epidemic.
When it comes to HIV sexual transmission the CDC says, “[p]eople living with HIV who take HIV medicine as prescribed and get and keep an undetectable viral load have effectively no risk of transmitting HIV to their HIV-negative sexual partners.”
The agency carefully chose its wording. HIV transmission to a negative partner is extremely low with proper treatment. However, the agency cannot rule out the possibility that transmission can occur.
HIV is a Manageable, but Costly and Life-changing Disease
In 2018, HIV is considered a manageable disease. Many people no longer consider it the death sentence it was when the virus first took hold. Initial reports of the virus sent panic across the United States, prompting discrimination against everyone within perceived proximity of disease. To date, it’s estimated that around 39 million people worldwide have died from the disease.
Although the virus is no longer the death sentence it once was, it is still a life-altering disease. HIV patients will be on some sort of medication for the rest of their lives. To keep viral loads undetectable, HIV-positive people need to adhere to a strict antiretroviral therapy regimen. Depending on whether or not a patient has medical insurance or access to proper healthcare, the drugs may be extremely costly. The CDC estimates that the lifetime cost of an HIV infection about $379,668.
In the past, HIV medications were ineffective, incredibly toxic and made the people on them very sick. Additionally, some people took several pills or doses of liquid medications a day. Present day medications are much more effective, have fewer or less severe side effects, and most only require one pill a day. However, medication alone is not the only thing that impacts a person’s life. Newly diagnosed people have described going into severe depression. In fact, 4 percent of HIV/AIDS-related deaths are by suicide. Others describe a decreased quality of life because people are fearful of or have no interest in dating an HIV-positive person. While others describe living 30 plus years with the disease, losing friends and partners to the disease and being financially insecure because death never came.
Yes, the disease is manageable in terms of living a healthy life. But HIV-positive people continue to face quality of life challenges.
Does a person with an undetectable viral load have to disclose their status?
Despite medical advancements, many state HIV disclosure laws will still require someone with an HIV-positive result to disclose their status. In addition to TasP measures, an HIV-negative person in a relationship with a positive person can take steps to protect themselves from the infection. Because of this, even if the viral loads are undetectable and transmission chances are low to non-existent, state laws still require you to disclose your status.
Many states have criminal laws for an HIV positive person who fails to disclose his, her or their status before engaging in a sexual act. Whether or not you are undetectable is irrelevant in the eyes of the law. If you know your positive status, to protect yourself from legal consequences you must tell potential partners. More importantly, just because an HIV-positive person is on ART drugs, does not mean that they are undetectable. As mentioned, it takes about six months to achieve undetectable status on modern ART drugs. Further, doctors will need to run tests to verify an undetectable viral load. Doctors will also run follow-up tests every six months to ensure viral loads remain undetectable.
HIV transmission can occur in two instances while on antiretroviral therapy (ART) drugs:
- The HIV-positive partner started ART, but hasn’t achieved or maintained viral suppression; or
- The HIV-positive partner achieves viral suppression, but the ART regiment later fails, or the partner stops taking their medication.
If HIV transmission occurs and you did not disclose your status because you believed you were undetectable, depending on where you live, you could be held criminally responsible. Similarly, infecting another person is not the only way an HIV-positive person can end up in the courtroom. Knowingly engaging in a sexual act without status disclosure can lead to charges or civil lawsuits.
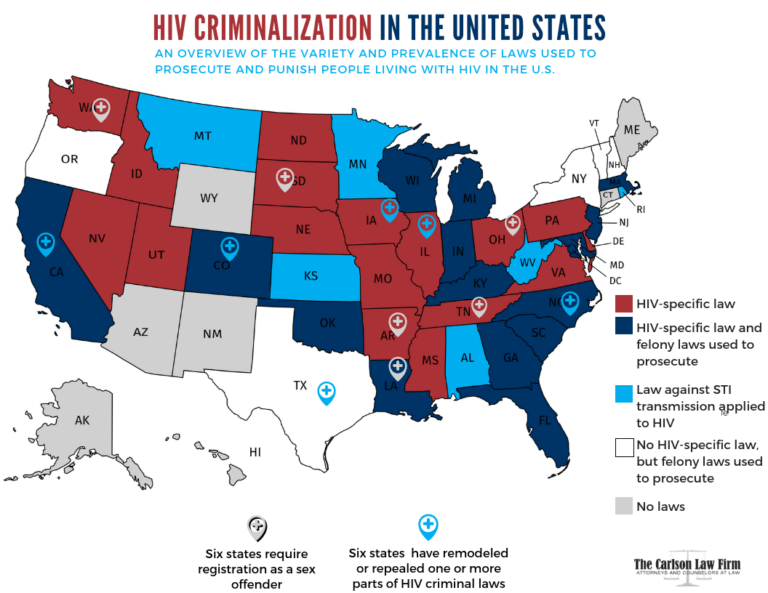
State HIV Disclosure Laws
There are varying degrees of HIV disclosure laws. Some states charge felonies for failures to disclose while HIV nondisclosure carries misdemeanor charges in others.
Legal Remedies for an Undisclosed HIV Infection
Depending on the state, knowingly transmitting an HIV infection to another person can end in a prison sentence. While criminal charges will punish wrongdoing, civil suits primarily focus on giving just compensation to a harmed person. An undetectable viral load is not a defense if a sexual partner somehow transmits HIV.
While HIV is no longer the death sentence it was 20-30 years ago. Antiretroviral therapy medications and doctors visits are incredibly expensive. This is why patients can seek monetary damages from those who transmitted the infection.
A Carlson Law Firm STD Contraction Lawyer Can Help
Finding out that you’ve contracted a sexually transmitted disease such as HIV can be life-shattering. Seeking justice may the first thought to pop into your head. However, filing an STD lawsuit is not as simple as many people believe. Proving liability in an STD lawsuit can be difficult. But this does not mean an STD contraction lawyer from The Carlson Law Firm is not up for the challenge.
We can help you in various ways:
- Pinpointing precisely who infected you may be difficult. This is particularly true if you have had more than one sexual partner in recent months. Furthermore, some people do not find out they have an STD for a long time. This makes it even more difficult to pinpoint the at-fault party.
- A person may be liable if they know about their condition and proceeded to have intercourse without disclosing the STD to his/her partner.
- Half the battle with these types of cases takes place even before a person contacts a lawyer. That is, many people who have contracted STDs can be embarrassed about bringing this type of information to loved ones, let alone a lawyer they have just met. The Carlson Law Firm is committed to complete client confidentiality as well as compassionate legal counsel.
Contact The Carlson Law Firm to get quality, confidential representation.





